Solutions
Payer Solutions
 |
Designing financial incentives to drive changeWe help payers design financial incentives to encourage plan members to achieve wellness objectives, including being physically active, losing weight, managing chronic conditions, and quitting smoking. We use behavioral economics to design incentive systems that provide the greatest impact at the lowest cost |
 |
Evaluating the effectiveness of ACOsWe help payers understand the effectiveness of their Accountable Care Organizations (ACOs) by assisting them in evaluating ACOs on multiple dimensions. We evaluate the relative likelihood of plan members attributed to ACOs to renew their plan memberships. Furthermore, he can evaluate the relative cost and quality of their care. |
 |
Evaluating the effectiveness of PCMHsWe help payers increase the effectiveness of their Patient-Centered Medical Homes (PCMHs). Using claims data, we help payers understand the factors that drive member cooperation with the PCMH initiative, identify complex patients at the point of care, and determine the PCMH-based providers best able to reduce emergency room utilization. |
 |
Evaluating regulatory complianceWe help payers perform the evaluations necessary to fulfill the requirements of state and federal regulators. Plans operating in the Managed Medicaid and Exchange-based markets are facing growing reporting requirements. We help plans work through the analysis process. |
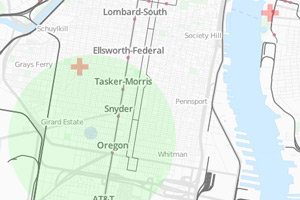 |
Determining whether networks provide sufficient accessWe help payers design networks that encourage in-network utilization by determining whether the networks provide sufficient access to care. We can estimate the travel times that members in different Census tracts experience when going to providers, enabling payers to assess whether narrow networks provide sufficient access. |
 |
Assisting decision makersWe help payer-based and state-based exchanges simplify the process through which individuals select their health plans. Given the wide number of options and variables, the task that individuals face can be daunting. Using principles from behavioral economics, We create systems to guide potential plan members through the selection process. |
Provider Solutions
 |
Predicting provider entry and exit from the marketWe help providers quantitatively predict the strategic responses of hospitals and ambulatory surgical centers (ASCs) to the entry and exit of service lines from their geographic markets. This service can be used by providers considering entry or exit from a service line or attempting to determine the impact of service changes by their competitors. |
 |
Predicting provider demandWe help providers determine the demand for specific surgical procedures in their service areas using patient-level data. Our demand estimates can be used by providers when applying for a Certificate of Need (CON) or assessing the potential of a market. |
 |
Measuring access to careWe help providers locate regions where there is inadequate access to time-sensitive procedures. Using information on hospitals’ schedules, combined with data on road networks and speed limits, We can estimate the travel times that patients experience when seeking care, and can show how access to care in different locations changes over the course of a day. |
 |
Estimating the cost of labor substitutionWe help providers estimate the cost of substituting physician extenders for physicians. A regulation restricting resident work hours created data that we can use to estimate the cost of offsetting reduced physician hours by hiring additional support staff. |
|
Reducing the impact of workload on hospital revenue
|
